Search

Innovative research aiming to prevent the spread of Strep A using ‘friendly’ bacteria in the throat has received a $1.5 million boost in the latest round of National Health and Medical Research Council grants.

Congratulations to four outstanding early-career researchers from The Kids Research Institute Australia, who have been awarded BrightSpark Foundation fellowships and project funding for 2026.
Perth investigators involved in a major global trial have launched an innovative Cultural Information Hub to maximise cultural safety for Aboriginal and/or Torres Strait Islander patients participating in research.

Whooping Cough Day in 2025 has a special significance to Catherine Hughes AM and her family - it marks a decade of dedication to vaccine advocacy after the loss of their four-week-old baby son Riley in 2015.

Eight outstanding researchers from The Kids Research Institute Australia and the Institute-led Broome STEM Festival are finalists in the 2025 Premier’s Science Awards.

Western Australian kids will have access to a needle-free nasal flu vaccine for the first time in 2026 as part of a new initiative to boost vaccination rates against the life-threatening virus.

Papua New Guinean researcher Dr Lincoln Timinao has been awarded the 2025 Deborah Lehmann Research Award (DLRA) for his work aimed at investigating the burden of malaria in young children.
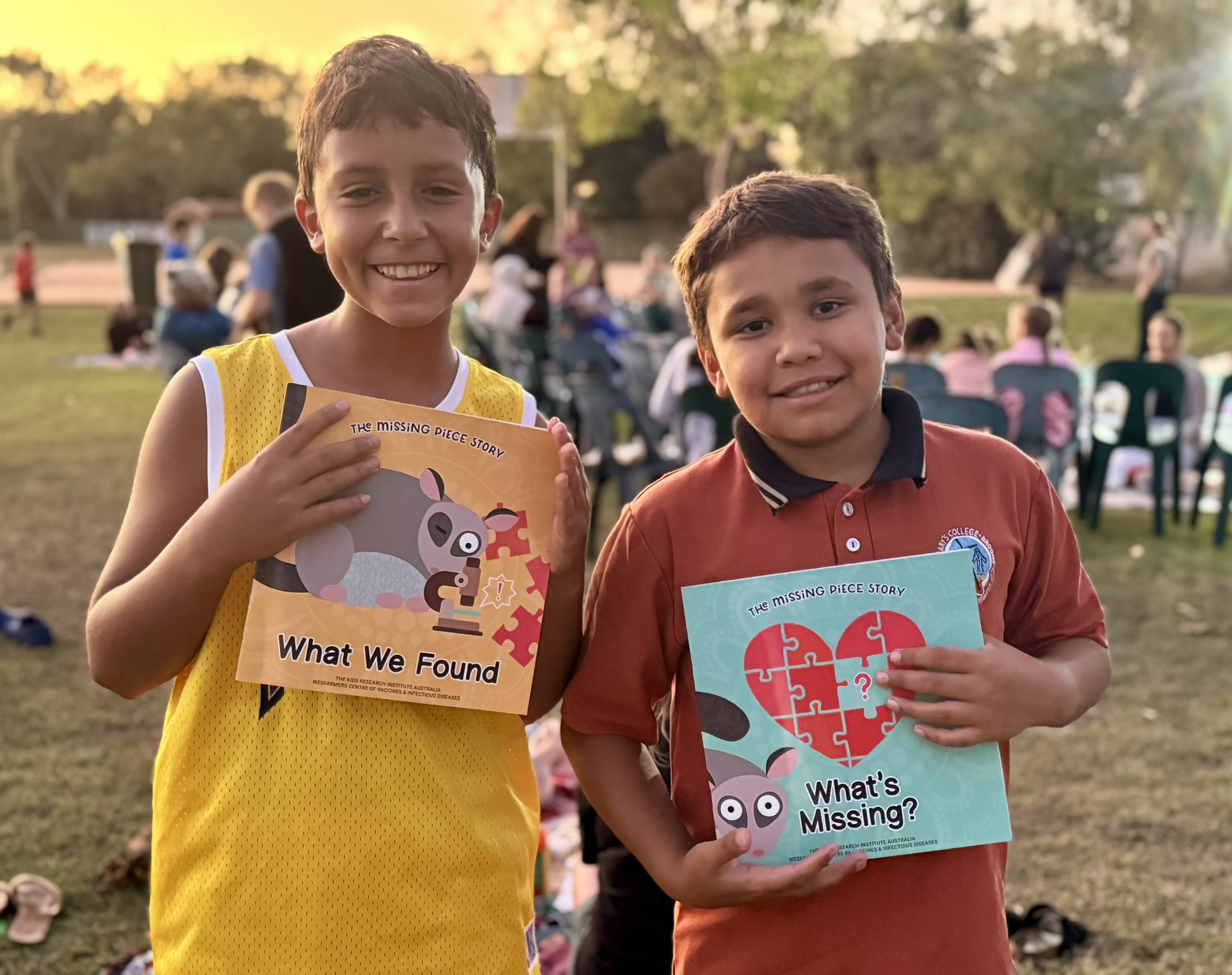
Wesfarmers Centre of Vaccines and Infectious Diseases researchers Dr Janessa Pickering and Dr August Mikucki travelled to Broome last week for the official launch of the long-awaited Missing Piece story books.

Free Family-Friendly Science Fun During National Science Week 2025. Get ready for an awesome adventure into the world of Science, Technology, Engineering and Mathematics!

National research led by the Wesfarmers Centre of Vaccines and Infectious Diseases, based at The Kids Research Institute Australia, has secured more than $3.4 million to assess the epidemiology of respiratory syncytial virus (RSV) throughout the country and optimise Australia’s immunisation strategy.
